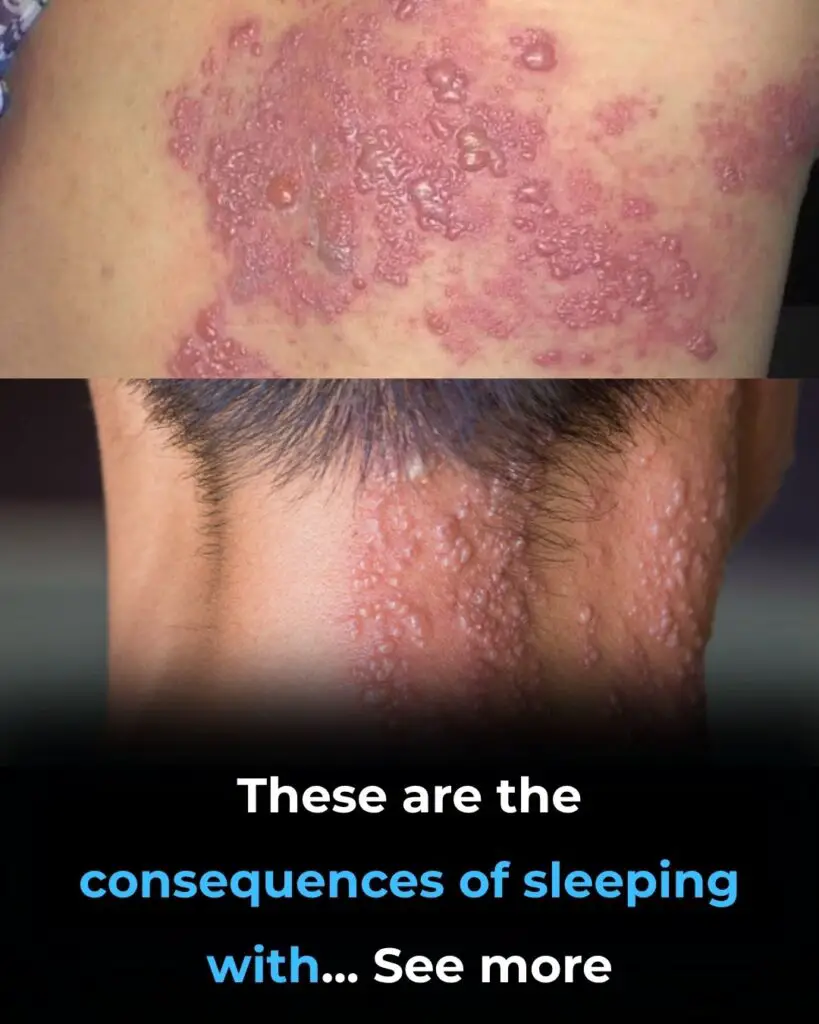
Human papillomavirus, commonly known as HPV, is far more common than most people realize. It is not rare, shameful, or a reflection of poor choices. In fact, medical experts agree that nearly every sexually active person will encounter at least one strain of HPV during their lifetime—often without ever knowing it.
Yet despite how widespread it is, confusion and stigma still surround HPV, especially when it comes to men and long-term consequences. Conversations often focus on women’s health, particularly cervical cancer, while overlooking how HPV affects everyone involved.
Understanding the real consequences of sleeping with someone who has HPV is not about fear. It is about clarity, prevention, and informed choices.
What HPV Actually Is
A common but misunderstood virus
HPV is not a single virus. It is a group of more than 200 related viruses, most of which spread through skin-to-skin contact during vaginal, anal, or oral sex. Because transmission does not require penetration or visible symptoms, the virus spreads easily and silently.
According to public health data, tens of millions of people are currently living with HPV, with millions of new infections occurring each year. Most people who have it do not feel sick and never develop symptoms.
Low-risk vs. high-risk strains
Not all HPV strains behave the same way. Some low-risk types cause genital warts, while others cause no symptoms at all and clear on their own. High-risk strains, however, can persist in the body and lead to serious health complications over time.
This distinction is important because many people carry HPV without knowing which type they have.
What Can Happen After Exposure to HPV
For women
Women face well-documented risks related to HPV. Persistent infection with high-risk strains is the primary cause of cervical cancer. HPV is also linked to cancers of the vagina, vulva, and anus.
Even when cancer does not develop, HPV can lead to abnormal cervical cell changes that require monitoring or treatment. These procedures, while often lifesaving, can be emotionally stressful and may affect fertility in certain cases.
Low-risk strains may cause genital warts, which are not life-threatening but can be uncomfortable and emotionally distressing.
For men
HPV affects men just as directly, even though it is discussed less often. Men can develop genital warts, penile cancer, anal cancer, and cancers of the mouth and throat linked to HPV.
Rates of HPV-related throat cancer have risen sharply in recent years, particularly among men. Many of these cases are connected to oral transmission of high-risk HPV strains.
Importantly, men can carry and transmit HPV without symptoms, meaning they may unknowingly pass the virus to partners.
Shared consequences for both partners
Because HPV often causes no immediate signs, partners may not know when or how transmission occurred. This uncertainty can strain relationships if misinformation or blame enters the conversation.
Understanding that HPV is common and often unavoidable helps reduce unnecessary guilt and fear.
How HPV Is Transmitted
More than intercourse alone
HPV spreads through intimate skin-to-skin contact. This includes vaginal sex, anal sex, oral sex, and genital touching. Condoms significantly reduce risk but do not offer complete protection because HPV can affect areas not covered by barriers.
This mode of transmission explains why HPV is so widespread and why even people with few partners can be exposed.
Why symptoms often go unnoticed
Most HPV infections are asymptomatic. There may be no pain, no visible warts, and no immediate health changes. The immune system clears many infections naturally within one to two years.
However, when the virus persists, it can quietly cause cellular changes that only show up later through screening or symptoms.
How to Reduce the Risks
Vaccination is the strongest protection
The HPV vaccine protects against the most dangerous strains of the virus, including those responsible for the majority of HPV-related cancers and genital warts. It is recommended for both males and females, ideally before sexual activity begins.
Young adults up to age 26 are encouraged to get vaccinated, and some adults up to age 45 may still benefit after discussing risks with a healthcare provider.
Vaccination protects individuals and reduces transmission across the population.
Safer sex practices help
Using condoms and dental dams lowers the risk of HPV transmission, even though it does not eliminate it entirely. Consistent use remains an important protective measure, especially for people with multiple partners.
Regular health screenings matter
For women, routine Pap tests and HPV screenings can detect abnormal cells early, long before cancer develops. Early detection dramatically improves outcomes.
For men, no standard HPV screening exists yet, but regular medical checkups and attention to unusual symptoms—such as persistent sores, warts, or throat issues—are essential. Men at higher risk should speak with healthcare providers about appropriate monitoring.
Addressing the Stigma Around HPV
Why shame does more harm than good
One of the greatest dangers surrounding HPV is silence. Many people feel embarrassed discussing it, which delays prevention, testing, and treatment.
HPV is not a moral failing. It does not mean someone was reckless or dishonest. It reflects the reality of human biology and intimacy.
Removing shame allows honest conversations, better protection, and healthier relationships.
Talking to a partner about HPV
If you or your partner has HPV, openness matters. Conversations should focus on facts, not blame. Sharing information, getting vaccinated if possible, and practicing safer sex are practical steps forward.
Calm, informed dialogue strengthens trust rather than weakening it.
What to Do If You or Your Partner Has HPV
If HPV enters your life, take these steps:
- Stay calm. Most infections resolve naturally.
- Learn which strain is involved, if possible.
- Get vaccinated if you are eligible.
- Attend regular medical screenings.
- Use protection to reduce transmission risk.
- Communicate openly with partners.
Knowledge and prevention are far more powerful than fear.
Final Thoughts
Sleeping with someone who has HPV does not automatically lead to serious illness. However, ignoring the facts can increase risks for both partners.
HPV is not a life sentence. It is a reminder that sexual health is shared health. Prevention, vaccination, screening, and honest conversation make a real difference.





Leave a Reply